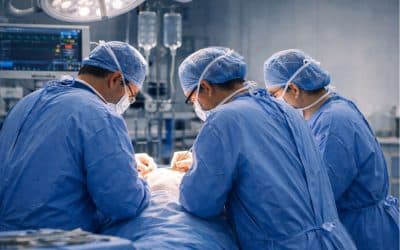
End of life, two conflicts around the notion of euthanasia
At a time when the law aiming to legalise euthanasia and assisted suicide under the term “assistance in dying”, is scheduled for its first reading by the Senate in January 2026, followed by a second reading at the National Assembly in February, two cases which have seen strong coverage in the media, have confirmed the level of sensitivity of the question of the end of life. They lead us to re-clarify according to the medical code of ethics, the narrow line separating therapeutic obstinacy and euthanasia.
The cases
In the hospital at Brive-la-Gaillarde, a conflict arose among the medical staff in the resuscitation department generating heated debate. The case was referred to the CFDT trade union by four of them, including two doctors, who then relayed their complaint against two of their doctor peers whom they accuse of “serious incidents” which could be considered as “euthanasia” on at least three patients. Against the backdrop of conflict within the medical team, the complaint regards the failure to comply with the LATA collegial protocol (Limitation and Termination of Active Therapies) and concerns several practitioners, over a period of around three years. The CFDT have reported the claim to the police and asked the hospital administration to “suspend” the doctors as a precaution. They are suspected of having euthanised patients, on the strength of unilateral decisions, i.e. with no collegial consultation.
At the Gustave Roussy Institute in Villejuif, a family has contested the decision – which this time was collegial – by the medical team to terminate the treatments of their loved-one, a man suffering from throat cancer and in a deep coma following several cardio-vascular accidents. The family won the case in the first instance and referred to the administrative court which, in September, ordered the patient to be maintained under artificial respiration. The hospital subsequently appealed to the State Council which ruled against the first instance magistrates and authorised the termination of treatment. According to it, the information provided by the family does not invalidate the advice of the medical team which considers that to maintain mechanical artificial respiration equates to “unreasonable obstinacy”. That is the term used to designate therapeutic obstinacy.
It is difficult to comment on each of these situations, due in particular to the lack of access to the respective medical records, it is however worth recalling a few elements of the medical code of ethics.
The mission of medical staff and its limits
The mission of a doctor is in all cases to provide care (and relief in particular), to attempt to cure, through “proportionate treatments”, without ever deliberately causing or hastening death, neither to do “everything” to avoid it, because death is the natural outcome of life. Euthanasia and assisted suicide (deliberately administered death) on the one hand, and ineffective or disproportionate treatments and artificially sustained life on the other hand are sent back-to-back.
The authority of the patient and its limits
How is the opinion of the “patient” taken into account? Not as a mere “customer”: because the medical staff are devoted to the health of the patient, not to the patient’s wishes. Doctors cannot however impose a treatment albeit useful or even vital: the enlightened consent of the patient or the patient’s person of confidence is always necessary prior to administering a treatment. Nor can the patient impose on the doctor to prescribe or administer a treatment which does not conform to medical practice and its code of ethics. The patient is not his/her own prescriber, nor are his/her next of kin, or person of confidence. That is the reason why advance directives are not binding, but merely “constraining”: doctors can deviate from them if they are “obviously inappropriate” or in the event of a vital emergency. Logic: Doctors in principle, have the competence to know what is best for the health of the patient.
Necessity and the limits of collegiality
Even if collegiality does in principle provide the advantage of preventing the potential unilateral omnipotence of a doctor, it cannot claim to represent an absolute ethical guarantee. First of all, because in an emergency, a doctor may be called upon to make a decision and to act alone; also and especially, since it is not because a decision is taken jointly that it is necessarily ethical. Experience has shown many “collective” decisions to be questionable. An unhealthy and complicit collegial decision may even result in a dilution of responsibilities.
The crucial criterion: intention
The criterion which must not be overlooked, and which remains crucial, concerns the intention of the act – or the intention which commands the abstention from acting.
There is a narrow dividing line between deliberately causing death and providing ineffective or disproportionate treatments.
It can be necessary to terminate ineffective or disproportionate treatments even if the possible, or foreseeable and inevitable consequence of such termination is death. It is the ethical principle of a double-effect act: death is not intended as such, but is accepted as a consequence of the termination of an ineffective or disproportionate treatment. The termination is compelled by the medical code of ethics in the name, in particular, of refusing to sustain life artificially. The criterion of intention is applicable to sedation: it must always be intended to provide relief, never to cause death. Deep and continuous sedation until death, combined with the termination of feeding and hydration, would amount to euthanasia if the intention is to cause death. Whence the need to comply with the recommendations published by the HAS (High Authority for Health) in 2018: on the basis of 8 criteria, they establish the difference between euthanasia and deep and continuous sedation until death.
It is quite true that the criterion of intention may appear subjective and difficult to verify. Nevertheless, it is the criterion used by the Court of Appeals, when seeking to qualify a death as: manslaughter or “violence resulting in death without such intention”; murder (with the intention of killing), or assassination, which assumes premeditation (the intention is pre-planned).
That is the context by which the above conflicts should be considered. Excesses appear in general when doctors (alone or as a team) take upon themselves to act in accordance with their subjective appreciation of the quality of life of the patient in the event of survival (for example the after-effects). Since that would amount to deciding that a life is not or is no longer worth living.
In principle, the very fact of stopping the operation of an artificial respirator for a patient in a coma (providing having maintained its operation for a reasonable length of time, having done everything possible to achieve recovery and having provided the opportunity of a return to spontaneous respiration) is not considered as euthanasia but rather the ending of artificially supported life. In such cases there is no question of a medical error or mistake which has placed the patient in such a situation.
The collegial procedure
That is precisely the purpose of the collegial procedure described in article R.4127-37-2 of the public health code, to secure the termination of treatments. The article describes how the doctor can decide and implement the termination of treatments, in accordance with the above-mentioned ethical principles:
- Consideration of the patient’s wishes expressed directly, via advance directives or through next of kin (initially by the person of confidence), information from the latter.
- Dialogue within the medical team with the additional advice of at least one other doctor who is not linked to the first hierarchically.
- Motivation of the decision by the deciding doctor who then informs the patient’s person of confidence or next of kin.
Whereas the law takes care – to reconcile the respect of patients, their next of kin and the medical teams – by establishing procedures where each has a role to play, these difficult situations reveal the absurdity or even inhumanity of the procedure for so-called “assistance in dying” as it is being considered by the bill currently being debated : the procedure is expeditious; the collegiality is stunted, since a doctor can unilaterally authorise the administration of death, following a limited and non-constraining consultation; and especially, the next of kin are completely ignored by the protocol : they are not invited to give an opinion ; it is not even specified that they must be informed.
Moreover, when considering the complexity and sensitivity of such medico-legal controversies surrounding the end of life, one can but point out the gravity of the claims put forward by
Dr. Didier Peillon, in his book « Ces malades que nous aidons à mourir » (These patients who we help to die), prefaced by the chief representative of ADMD (Association pour le Droit de Mourir dans la Dignité – Association for the right to die with dignity) which introduces him as a “Committed and fraternal doctor”. The doctor confesses to unilateral acts of euthanasia, which he decided alone, on the basis of his own appreciation, alone, under his authority as a doctor, therefore with no collegiality, and as the case may be, without the knowledge of the patient, or of his/her next of kin.
Suivez-nous sur les réseaux sociaux :